A Complete Guide to Proper Surgical Skin Prep Technique
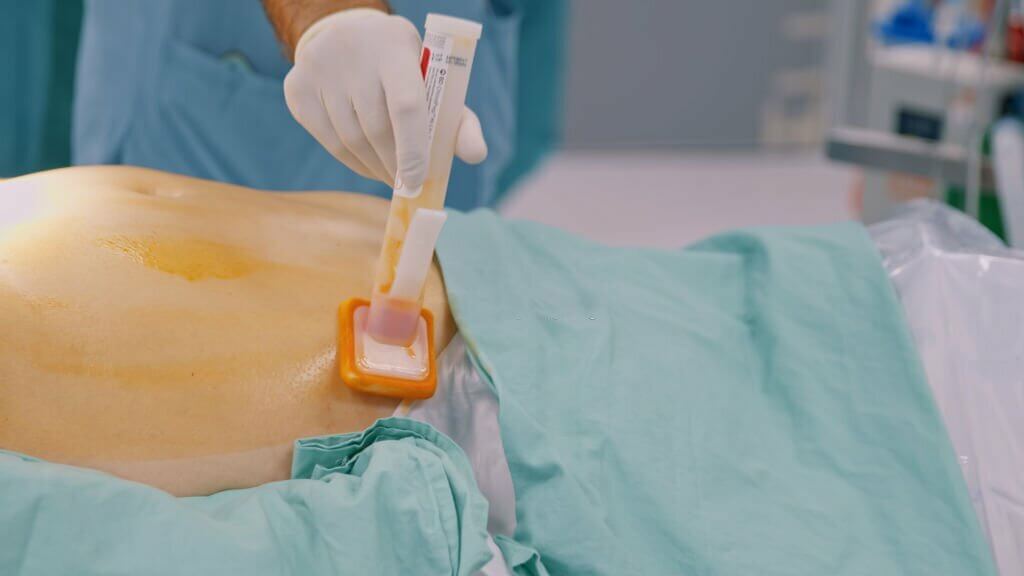
Surgical site infections (SSIs) are a major patient safety issue, causing increased morbidity, mortality, and healthcare costs. Appropriate surgical skin preparation is a critical step in reducing SSI risk. This article provides an overview of evidence-based best practices for preoperative skin preparation.
The Goal of Surgical Skin Preparation
The aim of surgical skin prep is to remove dirt, oil and transient microbes on the skin surface while rapidly killing resident skin flora at the incision site. This significantly reduces the microbial burden and risk of wound contamination during surgery.
The skin naturally hosts a diverse community of bacteria, fungi and viruses. Though harmless on intact skin, these microorganisms can cause devastating infections if introduced into surgical wounds. Thorough skin preparation is one of the most effective ways to prevent this.
Key Steps in Skin Preparation
-
1. Preoperative Cleansing
Patients should shower or bathe with plain soap on the night before or morning of surgery. This physically removes dirt, sweat, and some microbes. Antiseptic soaps provide no added benefit and may cause allergic reactions.
-
2. Hair Removal
Hair should be removed right before surgery using clippers with disposable heads. Avoid razors, as they cause microscopic cuts that encourage skin bacteria growth.
-
3. Skin Disinfection
Immediately before surgical incision, the skin should be disinfected with an alcohol-based chlorhexidine gluconate (CHG) or povidone-iodine (PI) antiseptic solution. This rapidly kills microorganisms and sustains antimicrobial activity on the skin.
-
4. Draping
After the antiseptic solution fully dries, the surgical site is draped. An iodophor-impregnated incise drape can help reduce skin recolonization during long procedures.
Choosing the Right Skin Disinfectant
Alcohol-based solutions are preferred because alcohol is highly antimicrobial and fast-acting. For mucosal or ophthalmic procedures, aqueous CHG or PI should be used instead to avoid tissue irritation.
2% CHG and 0.5% CHG solutions have similar efficacy. As repeated exposure to 2% CHG can cause allergic reactions, the 0.5% concentration is preferred for most procedures.
Though both effective, CHG has longer-lasting activity than PI. Some data also suggests CHG may prevent more SSIs compared to PI. Both antiseptics are inactivated by blood or bodily fluids.
Proper Surgical Skin Prep Technique
-
1. Use a back-and-forth motion when applying the antiseptic, covering the incision site and surrounding area.
-
2. Allow the solution to fully dry before draping - this takes at least 2 minutes for alcohol-based products.
-
3. Open applicator ampules aseptically and discard after single-patient use to prevent contamination.
-
4. Add sterile dye to CHG solutions so the prepped area is easily visible.
-
5. Handle potentially flammable alcohol-based preparations cautiously, allowing complete drying before draping.
-
6. Follow manufacturer instructions for application volumes and drying time.
Proper skin antisepsis technique ensures maximum antimicrobial efficacy and prevention of SSIs. Adhering to evidence-based protocols and selection of appropriate solutions improves patient outcomes.
The Mantacc CHG Applicator
The Mantacc CHG applicator contains 2% chlorhexidine gluconate and 70% isopropyl alcohol - a proven combination for broad-spectrum skin disinfection. The sterile polyurethane foam head optimizes skin contact and antiseptic delivery. Mantacc applicators come individually wrapped for aseptic single-patient use. Consider integrating this highly-effective CHG prep solution into your surgical skin preparation protocol.
Click to View → Mantacc MCA-T260 26ml CHG Applicator
Related Posts
Everything You Need To Know About CHG Swabsticks
Ethanol vs Isopropyl Alcohol: Which Works Better With CHG Applicator For Skin Preparation?
The CHG Applicator: Championing Effective Skin Preparation
Why is CHG Solution Better Than Iodine For Reducing CRBSIs?