News and Blogs
Patient Experiences with NP Swabs

Nasopharyngeal (NP) swabs play a critical role in specimen collection for various diagnostic tests, particularly for detecting respiratory infections such as influenza, COVID-19, and other viral illnesses. These swabs are designed to collect samples from the nasopharynx, a region in the upper part of the throat behind the nose. The collected samples are then processed and analyzed in a laboratory to diagnose infections, helping healthcare professionals make informed decisions regarding patient care and treatment.
Given the widespread use of NP swabs for diagnostic purposes, it is vital to ensure the accuracy and reliability of the collected samples. One of the key factors influencing the quality of specimen collection is patient comfort and compliance. When patients are at ease during the swabbing process, they are more likely to cooperate and comply with the procedure, resulting in a higher likelihood of obtaining an adequate sample for analysis.
Patient comfort is essential for multiple reasons. Firstly, an uncomfortable or painful experience can discourage patients from undergoing future diagnostic testing, which could result in delayed or missed diagnoses. Secondly, patient discomfort may lead to involuntary reflexes, such as coughing, sneezing, or moving during the swabbing process, which could compromise the integrity of the collected sample. Inadequate or contaminated samples can, in turn, lead to false-negative or inconclusive test results, undermining the accuracy of diagnostics and hindering appropriate patient care.
Patient compliance is also crucial for accurate diagnostics. A cooperative patient is more likely to follow the healthcare professional's instructions during the procedure, increasing the chances of successful sample collection. Ensuring patient compliance often involves providing clear explanations about the importance of the test, addressing any concerns or fears, and offering reassurance throughout the process.
I. Common Patient Concerns and Discomforts with NP Swabs
Nasopharyngeal swabs are used to collect samples from the back of the nose and throat to test for COVID-19. However, the collection procedure for NP swabs can cause discomfort and require trained healthcare staff to perform. Saliva and self-administered nasal (SN) swabs are, in many ways, ideal alternatives to NP swabs. Issues include incorrect angling of the swab and inappropriate depth of insertion. If the swab angle is too high, a puncture may occur. The sinuses can protect the skull base to a degree, Dr. Chen said. Injury from incorrect nasopharyngeal swab technique, while rare, may include cerebrospinal fluid leakage or severe bleeding.
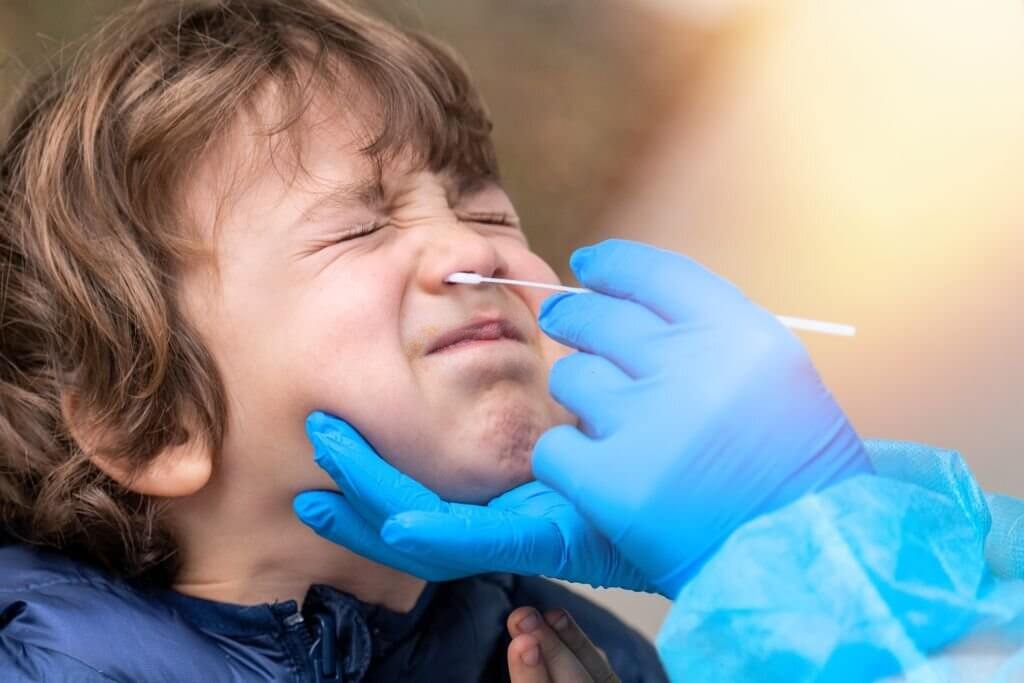
The insertion of a swab into the nasopharynx can cause discomfort and pain for some patients. This discomfort often results from the swab making contact with the sensitive nasal tissues and the nasopharyngeal wall. Patients may feel a stinging or burning sensation as the swab is inserted, and some may even experience watery eyes or a brief sensation of pain. Healthcare professionals can minimize this discomfort by using proper swabbing techniques and ensuring that the swab is inserted gently and smoothly.
During nasopharyngeal swabbing, some patients may experience a gag reflex, leading to discomfort and anxiety. This reflex can be triggered when the swab comes into contact with the soft tissues at the back of the throat or the nasopharynx. To minimize the risk of triggering the gag reflex, healthcare professionals should instruct patients to relax, breathe through their mouths, and tilt their heads back slightly during the procedure. Additionally, using swabs with a smaller diameter or more flexible materials can help reduce the likelihood of inducing a gag reflex.
Patients may be concerned about the accuracy of the specimen collection, fearing that improper swabbing could lead to false-negative or inconclusive test results. To alleviate these concerns, healthcare professionals should provide clear explanations about the swabbing process and its importance for accurate diagnostics. They should also reassure patients that they are trained in the proper techniques for specimen collection and will take all necessary precautions to ensure the sample is collected correctly.
II. Strategies for Improving Patient Comfort during NP Swab Collection
Implementing strategies to improve patient comfort during nasopharyngeal swabbing can enhance patient compliance and contribute to more accurate diagnostic results. By focusing on proper techniques, positioning, distraction, and the choice of swabs, healthcare professionals can create a better experience for patients undergoing this essential diagnostic procedure.
Using the correct technique for swab insertion and rotation is crucial for minimizing patient discomfort. Healthcare professionals should gently insert the swab along the nasal floor, parallel to the palate, to avoid causing unnecessary pain. Once the swab reaches the nasopharynx, a gentle rotation should be performed to ensure adequate sample collection. Proper training in these techniques can help reduce discomfort for patients and ensure the collection of high-quality samples.
The patient's position during the swabbing process can significantly impact their comfort level. Healthcare professionals should ensure that patients are seated comfortably and encourage them to relax their facial muscles. Tilting the head back slightly can also help open the nasal passage, making it easier to insert the swab and reducing the risk of injury to the nasal tissues.
Distraction techniques can help patients focus on something other than the swabbing process, reducing anxiety and discomfort. Healthcare professionals can engage patients in conversation, encourage deep breathing exercises, or suggest that patients visualize a relaxing scene. These techniques can help patients feel more at ease during the procedure and improve their overall experience.
The choice of swab material can significantly impact patient comfort during nasopharyngeal swabbing. Swabs made from softer or more flexible materials can reduce discomfort by conforming to the nasal passage's shape and minimizing irritation to the sensitive nasal tissues. Healthcare professionals should consider using swabs with these features to enhance patient comfort and encourage compliance during the specimen collection process.
III. Enhancing Patient Compliance during Specimen Collection
Enhancing patient compliance during specimen collection is crucial for obtaining accurate test results and maintaining a smooth workflow in laboratories. Based on the provided web search results, several strategies can be employed to improve patient compliance during specimen collection:
- 1. Improved communication and collaboration between laboratory and healthcare professionals: Clear communication between laboratory staff and healthcare professionals can help ensure that the specimen collection process is well understood by both parties. This can lead to better instructions being given to patients, which in turn can result in increased patient compliance.
- 2. Education and training of healthcare staff responsible for specimen collection: Ensuring that healthcare staff are properly trained and educated on specimen collection procedures is critical . Staff should be knowledgeable about the correct methods and materials for collecting specimens, as well as the importance of maintaining a sterile environment. This will enable them to confidently guide patients through the process and address any concerns or questions.
- 3. Audit and feedback of labeling errors and real-time event reporting: Regular audits and real-time feedback of any errors or issues during specimen collection can help identify areas for improvement and ensure corrective measures are implemented. This proactive approach can lead to a more streamlined and efficient collection process, ultimately improving patient compliance.
- 4. Implementation of new technology: The use of modern technology can help streamline the specimen collection process and reduce the risk of errors. For instance, electronic ordering systems and barcoding technology can minimize human error, ensuring the correct specimens are collected and accurately labeled.
- 5. Clear instructions and guidance: Providing patients with comprehensive instructions and guidance on the specimen collection process can significantly improve patient compliance. For example, including a completed Test Request form with each patient specimen can help clarify the required tests and ensure patients understand the steps involved in the collection process.
IV. Training Healthcare Professionals for Improved Patient Experience
Training healthcare professionals for an improved patient experience is essential in today's healthcare environment. Enhancing the patient experience is one of the Quadruple Aim objectives in healthcare, along with improving population health, reducing costs, and improving the work-life of clinicians and staff. The patient experience is the sum of all interactions that influence patient perceptions across the continuum of care.
To train healthcare professionals effectively for an improved patient experience, the following strategies can be considered:
- 1. Recognize patients as consumers: Healthcare professionals should be trained to view patients as consumers, understanding that they have choices and preferences in their care. This perspective encourages providers to treat patients with respect and to strive for excellence in service delivery.
- 2. Emphasize effective communication: Training healthcare professionals in effective communication can help build trust, understanding, and empathy between patients and providers. This includes active listening, clear explanations, and tailoring communication to suit the individual patient's needs and preferences.
- 3. Teach patient-centered care: Encourage healthcare professionals to adopt a patient-centered approach, which involves understanding and respecting the unique needs, preferences, and values of each patient. This can lead to more personalized care plans and a better overall experience for the patient.
- 4. Enhance teamwork and collaboration: Training healthcare professionals to work effectively as a team can lead to better coordination and integration of care, ultimately improving the patient experience. Interprofessional education and team-based training programs can help foster collaboration and communication between different healthcare providers.
- 5. Promote cultural competency: To provide equitable care, healthcare professionals should be trained in cultural competency, which involves understanding the diverse cultural backgrounds of patients and tailoring care to meet their specific needs. This can help reduce health disparities and improve the overall patient experience.

Ensuring patient comfort and compliance during nasopharyngeal swab collection is crucial for accurate diagnostics and improving overall healthcare outcomes. The key strategies for enhancing the patient experience include using proper techniques, ensuring the patient is in a comfortable position, employing distraction techniques, and selecting swabs with softer or more flexible materials. Furthermore, healthcare professionals should focus on empathetic communication, regular training, and staying up-to-date with new developments in swab design and techniques.
As a leading manufacturer of sample collection and transport systems, Mantacc bears a significant responsibility in this endeavor. By consistently producing high-quality, comfortable, and reliable nasopharyngeal swabs, Mantacc plays a vital role in facilitating accurate diagnostics and improved patient experiences. Moreover, Mantacc can contribute to the ongoing education of healthcare professionals by offering resources, guidelines, and best practices for NP swab collection.
By understanding the importance of patient comfort and compliance, and working collaboratively with healthcare professionals, Mantacc can continue to lead the industry in providing innovative and effective solutions for specimen collection, ultimately contributing to better patient care and more accurate diagnostic results.
Click to View → Mantacc Nasopharyngeal Swab Collection
References
- 1. Saliva is more sensitive than nasopharyngeal or nasal swabs for diagnosis of asymptomatic and mild COVID-19 infection
- 2. COVID-19 nasal swab test may not be best for those who've had sinus surgery
- 3. Getting It Right for Patient Safety: Specimen Collection Process Improvement From Operating Room to Pathology
- 4. Specimen Collection and Preparation Guide
- 5. Advancing Standards for Specimen Labeling and Tracking
Related Posts
NP Swabs: The Gold Standard Sampling for Respiratory Infections
How to Obtain a Nasopharyngeal Swab Specimen
Nasopharyngeal Swab vs Oropharyngeal Swab: Which is Better In Specimen Collection?






