News and Blogs
Everything You Need To Know About Cervical Specimen Collection
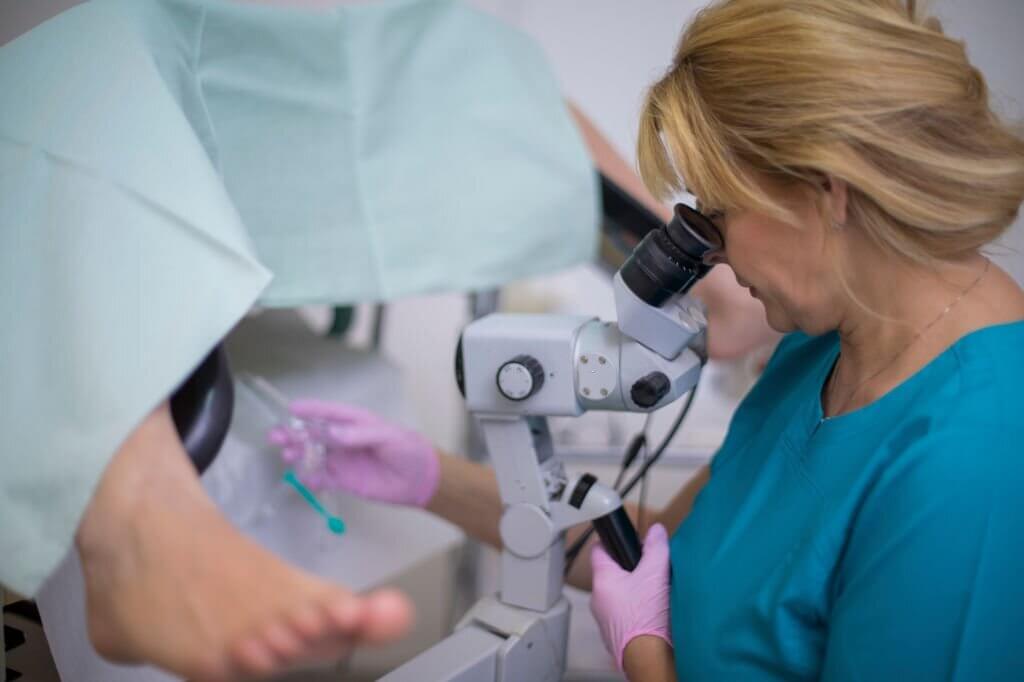
Cervical cancer screening through tests like the Pap smear and HPV test are vital prevention tools all women should utilize. Regular screening allows for the detection of abnormal cervical cells and HPV infection before they potentially develop into cancer. While screening procedures have improved dramatically over the years, specimen collection remains a necessary first step. Pap and HPV tests require a sample of cervical cells to be collected during a pelvic exam. This introductory section will provide background information on cervical cancer screening and an overview of cervical specimen collection methods and guidelines. The goal is to educate readers on the importance of this routine procedure and empower women to take charge of their reproductive health.
I. When to Get Tested
Knowing when to start cervical cancer screening and how often to repeat it is crucial for early detection and prevention. Current guidelines recommend that women begin regular Pap test screening at age 21. Between ages 21-29, guidelines advise getting a Pap test every 3 years. For women ages 30-65, the preferred recommendation is to get both a Pap and HPV test every 5 years, or a Pap test alone every 3 years. However, screening recommendations may vary based on individual risk factors and medical history.
Women who are HIV-positive, have a weakened immune system, were exposed to diethylstilbestrol (DES) before birth, or have had previous abnormal screening results may need more frequent testing. This section provides an overview of the latest age-based cervical cancer screening recommendations from leading health organizations. Understanding when to start testing and how often it needs to be repeated empowers women to take charge of their reproductive health.
II. Types of Cervical Specimen Collection
There are two main types of screening tests used for the early detection of cervical cancer and abnormalities - the Pap test and the HPV test. The Pap test, also known as a Pap smear, involves collecting a sample of cells from the cervix to examine under a microscope for signs of precancerous changes. The HPV test detects infection with high-risk strains of the human papillomavirus that could lead to cervical cancer if left untreated.
While both the Pap and HPV test require collecting a cervical cell sample, there are some key differences. Pap tests aim to find precancerous cell changes, while HPV tests look for the virus that causes these cell changes. Pap tests require a visual exam of the cervix, while HPV tests can use self-collected vaginal samples. Understanding the variations between these screening tests allows women to make informed decisions about their cervical cancer prevention plan.
III. How Specimen Collection is Done
Getting a clear understanding of the step-by-step process can help ease anxiety about cervical specimen collection. The procedure is typically performed during a pelvic exam at your doctor's office. First, you'll lie down on the exam table and a speculum will be inserted to open the vagina and expose the cervix. Using a small brush or spatula, a sample of mucus and cells will be collected from the cervix.
For a Pap test, the sample is smeared onto a glass slide and sent to a lab for microscopic examination. For an HPV test, the sample is preserved in a vial and analyzed for the presence of viral DNA. The actual cell collection only takes about 10-60 seconds. While there can be some discomfort from the speculum, the brushing feeling is usually mild. Knowing what to expect can make the experience less intimidating. Your healthcare provider will guide you through each step and answer any questions.
IV. Self-Collection Options
Some screening options allow women to collect their own cervical sample in the privacy of home rather than visiting a clinic. HPV testing can be performed on self-collected vaginal swabs. Self-sampling kits typically consist of a swab, instructions, and a tube or envelope to mail the sample to a lab. Benefits include convenience, privacy, and avoiding the anxiety of a clinical setting. However, there are some limitations. Self-collected samples may not provide as high quality of a sample as clinician-collection. HOME instructions must be followed precisely to ensure usefulness of the sample. And self-sampling is not yet approved for primary Pap tests, only as a follow-up to abnormal results. Discussing the pros and cons of self-sampling with your provider can determine if it may be an appropriate cervical screening method for you.
V. Test Results
The cervical cells collected during the Pap smear or HPV test are preserved and transported to a cytology lab. Trained experts analyze the preserved cells under a microscope to detect any abnormal changes.
Understanding your test results is crucial for determining any needed follow-up care. A “normal” Pap test means no abnormal, precancerous cervical cells were detected. An “abnormal” result means precancerous changes were identified that require further testing. An abnormal Pap result may lead to repeat testing in 6-12 months or referral for a colposcopy biopsy to examine the cervix in greater detail. For HPV tests, a “positive” result means detection of a high-risk strain and the need for repeat testing.
HPV infections often clear on their own, but persistent infection is linked to cervical cancer. Close follow-up care is key to treating detected abnormalities before they potentially progress. While an abnormal result may be unsettling, keep in mind that early detection through screening is the best way for cervical cancer to be prevented and treated successfully.
VI. Reducing Discomfort
While usually quick, cervical sample collection can cause some temporary discomfort or anxiety. There are techniques you can use to help relax and minimize any pain. Focusing on deep, slow breathing is key. You may also find it helpful to apply a numbing gel on the cervix prior to the procedure. During the exam, concentrate on your breathing and a peaceful image rather than tensing up. Use affirming self-talk reminding yourself “I am safe” and “this will be over soon.” To reduce cramping, take ibuprofen an hour before your appointment. Your provider can also adjust the position, angle, and device used based on feedback to find the most comfortable approach. Being open about any discomfort allows adjustments to be made so the procedure can be completed smoothly.
VII. What are the symptoms of sexually transmitted diseases (STDs)?
Many STDs do not produce obvious symptoms, so it is possible to have an infection without being aware of it. Some common signs of STDs can include sores, bumps, warts, rashes, itching, or burning in the genital area. Abnormal discharge from the penis or vagina is another symptom. Pain or discomfort during sexual intercourse is also a potential indicator of infection. For women, pelvic pain, bleeding between periods, and pain while urinating can signal an STD. Flu-like symptoms like fever, chills, body aches, or swollen glands can accompany some STDs. However, the only way to know for sure is to get tested, as relying on symptoms alone is not sufficient for diagnosis. Getting regularly tested for STDs is important for one's sexual health, even without symptoms present.
Staying up-to-date on cervical cancer screening is the best way for women to take charge of their health. While getting tested can feel daunting, understanding the guidelines, procedures, and options helps transform it into an empowering act. Cervical specimen collection through Pap and HPV testing is a quick, simple, and vital routine. Products like Mantacc's cervical kits can help streamline the process to make it easy, accurate, and comfortable. Discuss your screening options with your provider to decide what works best for your health profile. Whatever method you undergo, be sure to get tested regularly! Catching abnormalities early is key to preventing cervical cancer through this life-saving care. With the right information and tools, screening can be stress-free.
Related Posts
Specimen Collection and the Ongoing Battle Against Tuberculosis in Indigenous Populations
The Science of Detection in Forensic Drug Testing and Specimen Collection Methods
A Comprehensive Guide to Specimen Collection for Gastrointestinal Pathogen Detection
Nasopharyngeal Swab vs Oropharyngeal Swab: Which is Better In Specimen Collection?
What is An Effective Specimen Collection and Transport System?







